When you incur high medical care costs
Your copayment for medical care costs is capped. If your copayment calculated based on certain standards exceeds the maximum, the excess amount will be paid as "High-Cost Medical Care Benefits".
By using a Myna health insurance card, you will be exempt from payments beyond the maximum copayment amount under the High-Cost Medical Care Benefits system without any prior procedures.
We recommend using a Myna health insurance card. Using this card will eliminate the need to apply in advance for a Certificate of Application of Maximum Copayment Amount.
- High-Cost Medical Care Benefits
- If you want to make sure the amount you pay at the reception desk of the hospital will not exceed the Cost-Sharing Maximum Amounts(Application of Maximum Copayment Amount)
- How High-Cost Medical Care Benefits are calculated
- If your copayment is reduced still further
- Description
- Procedures
- FAQ
High-Cost Medical Care Benefits
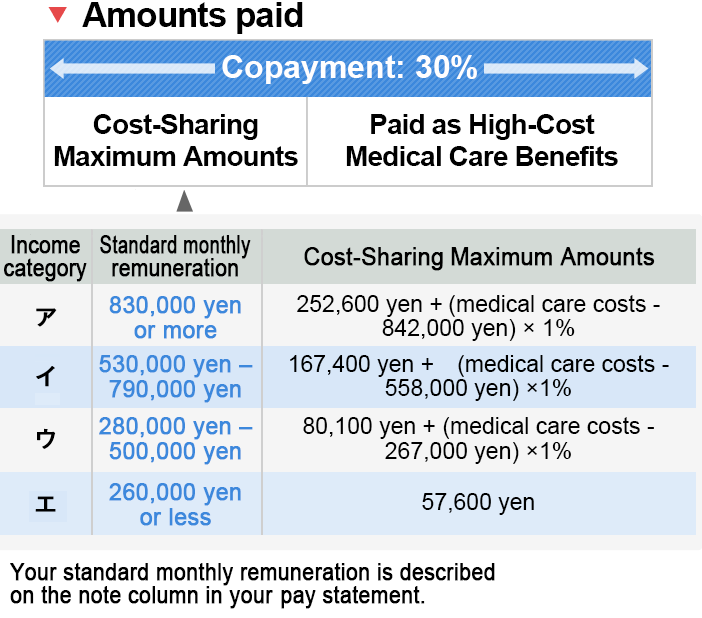
- ** Meal expenses, accommodation expenses, and charges of beds incurring an extra charge during hospitalization are not eligible for High-Cost Medical Care Benefits.
- ** See here for Cost-Sharing Maximum Amounts for persons aged 70-74.
- ** See here for Cost-Sharing Maximum Amounts for persons with low income.
If the copayment amount for medical care costs paid at the reception desk of the hospital becomes high, the Health Insurance Association will automatically pay the amount beyond a certain amount later (the Cost-Sharing Maximum Amount) to help ease the burden of medical care costs. This is referred to as “High-Cost Medical Care Benefits.”
High-Cost Medical Care Benefits are calculated for medical care costs incurred over a one-month period, from the first through the last day of the month. High-Cost Medical Care Benefits are also calculated on a per-person, per-hospital (outpatient/inpatient, medical/dental, etc.) basis.
If you want to make sure that the amount you pay at the reception desk of the hospital will not exceed the Cost-Sharing Maximum Amounts
By using your Myna health insurance card, you can ensure that the amount you pay will not exceed the Cost-Sharing Maximum Amount, without completing the following procedures.
Note that you will need a Certificate of Application of Maximum Copayment Amount in the following cases. If you need this certificate, apply in advance.
- When not using a Myna health insurance card
- Examinations and treatment received at a medical care institution or other facility that has not adopted the online eligibility verification system
- When not using a Myna health insurance card and you are 70 or older and in the same income category as active workers Ⅰ or Ⅱ
- * Even when using a Myna health insurance card, those in the low-income category must apply in advance for a Maximum Copayment/Reduced Standard Copayment Certificate to be treated as falling in the low-income category.
By showing this “Certificate of Application of Maximum Copayment Amount” to the medical care institution, you can ensure that the amount of medical care costs for which the hospital bills you (per month) will not exceed the Cost-Sharing Maximum Amount and reduce the amount of medical care costs you must pay at the hospital on any single visit (You can use this certificate for both inpatient and outpatient care).
Prior application required
“The Certificate of Application of Maximum Copayment Amount” is used to confirm your income category. You must apply to the Health Insurance Association in advance for this Certificate.
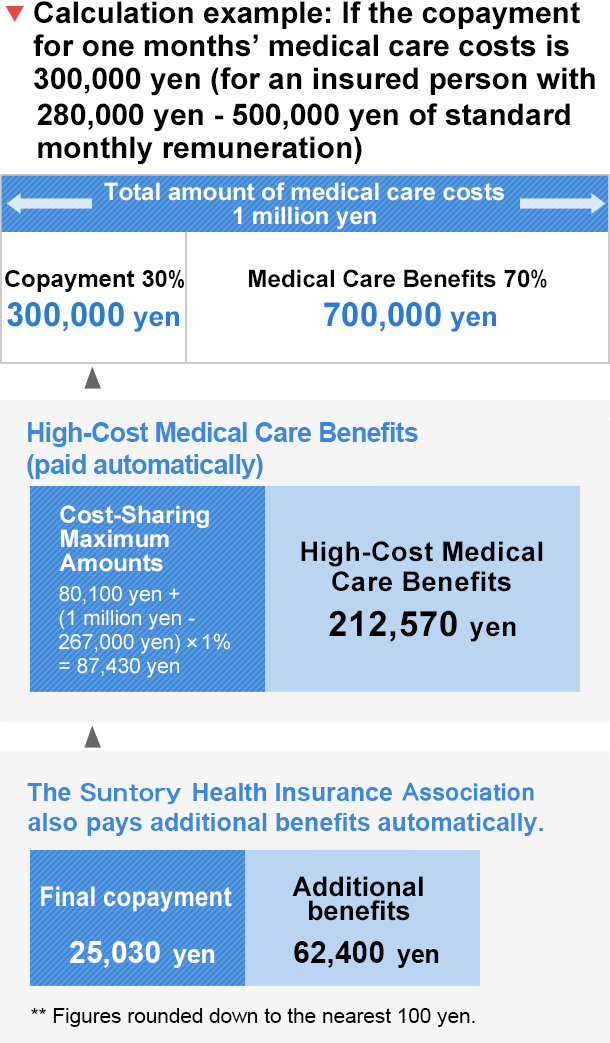
How High-Cost Medical Care Benefits are calculated
- If you become sick or are injured
- ■ Medical Care Benefits
- ■ Additional benefits
- ■ Meals during hospitalization
If your copayment is reduced still further
You can combine copayments for an entire household (Total High-cost Medical Care Benefits)
Even when the copayment for one case for one month is less than the maximum, if members of the same household have made copayments of 21,000 yen and its payments are more multiple times in the same month, they can combine those amounts for the purposes of the Cost-Sharing Maximum Amount.
If the total amount exceeds the Cost-Sharing Maximum Amount, then the excess amount is paid by the Health Insurance Association as “Total High-cost Medical Care Benefits”.
The SUNTORY HEALTH INSURANCE ASSOCIATION also pays as additional benefits the Cost-Sharing Maximum Amounts minus 25,000 yen per person.
The Cost-Sharing Maximum Amount will be reduced for frequent qualification of expenditures.
If a single household qualifies for High-Cost Medical Care Benefits three or more months in a single year (the most recent 12 months), the Cost-Sharing Maximum Amount will be reduced to the amount of the table below starting with the fourth month.
| Standard monthly remuneration | Cost-sharing maximum amounts |
|---|---|
| 830,000 yen or more | 140,100 yen |
| 530,000 yen - 790,000 yen | 93,000 yen |
| 280,000 yen - 500,000 yen | 44,400 yen |
| 260,000 yen or less | 44,400 yen |
Those receiving treatment for specified diseases and disorders
The amount paid to the medical care institution will not exceed 10,000 yen per month for patients with haemophilia, patients with AIDS receiving antiviral drugs, and patients with chronic nephritis who require artificial dialysis for an extended period, if they have been certified as having specified diseases and disorders.
However, if a patient requiring artificial dialysis and under 70 years of age qualifies as a person with 530,000 yen or more of standard monthly remuneration, his or her copayment will be 20,000 yen/month.
If you are eligible, apply for issue of Certificates Issued for Specific Disease Treatment.
Caution
The right to claim health insurance benefits expires in two years.
There is no frequently asked questions and answers that have been registered.






